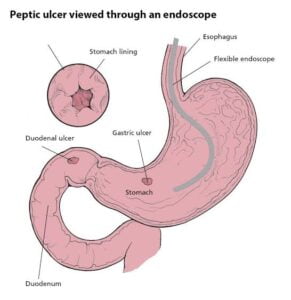
Peptic ulcer disease causes open sores in your stomach lining or duodenum (the top of your small intestine). Symptoms include burning or gnawing stomach pain. Treatment is with medications, unless you have complications like bleeding. There are two main causes. You’ll need a diagnosis to make sure you’re treating the right cause.
Overview
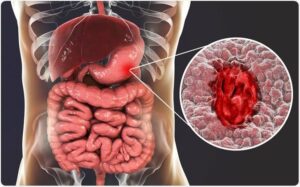
What is peptic ulcer disease?
Peptic ulcer disease is a condition that causes ulcers (open sores) to develop in the lining of your digestive tract. “Peptic” means it’s related to digestion. The word is derived from pepsin, the major digestive enzyme that your stomach produces.
Pepsin and stomach acid are the active ingredients in your stomach juices that help to chemically break down food for digestion. Some of these juices also pass into the first part of your small intestine (duodenum). By design, these juices are highly corrosive.
All of your gastrointestinal tract has a protective mucous lining that insulates it from the substances inside. It’s especially strong in your stomach and duodenum. But in peptic ulcer disease, this protection fails, and digestive juices corrode through the lining.
An ulcer is an erosion that penetrates through all three layers of the mucous lining (mucosa). Most peptic ulcers occur in your stomach or duodenum, where gastric juices are most active. Less commonly, they can also occur elsewhere in your GI tract.
What are the different types of peptic ulcers?
Peptic ulcer disease most often affects your stomach and duodenum.
- Duodenal ulcers account for almost 80% of peptic ulcers.
- Stomach ulcers account for almost 20% of peptic ulcers.
You can get a peptic ulcer elsewhere in your gastrointestinal tract under unusual circumstances that cause stomach juices to pass through those parts. For example:
- Esophageal ulcer. Chronic acid reflux, stomach acid rising into your esophagus, may eventually erode the mucous lining in your esophagus enough to cause an ulcer. Your esophagus lining isn’t as protected against acid as your stomach lining is.
- Jejunal ulcer. You can get an ulcer in your jejunum, the middle part of your small intestine, as a side effect of surgery connecting your stomach to your jejunum (gastrojejunostomy). This is also called a stomal ulcer, marginal ulcer or anastomotic ulcer.
How common is peptic ulcer disease?
Between 5% and 10% of people worldwide will develop peptic ulcer disease (PUD) in their lifetimes. It can develop at any age, though it’s more common in middle-aged adults. It’s also more common in people assigned male at birth (AMAB) than in people assigned female at birth (AFAB).
Symptoms and Causes
What are peptic ulcer symptoms?
Up to 70% of people with peptic ulcer disease don’t notice any symptoms. But the most common symptoms people report are epigastric pain (central upper abdominal pain) and indigestion (dyspepsia). These symptoms come and go persistently.
Indigestion describes a combination of symptoms that occur after eating and during digestion. It includes epigastric pain with a notable burning quality, combined with a feeling of fullness that comes on shortly after eating and/or lasts a long time after.
This burning sensation is the feeling of stomach acids and enzymes eating through your gastrointestinal lining. Some people also describe it as a “gnawing” sensation. You may be able to locate it in a particular spot (“focal” abdominal pain).
You may not be able to tell if the ulcer is in your stomach or duodenum. But some clues can help you tell. For example, a stomach ulcer will often feel worse shortly after a meal (within 30 minutes), when gastric juices are at their peak.
On the other hand, a duodenal ulcer may feel better shortly after a meal. But you’ll feel it more about two to three hours later, when the food and digestive juices enter your duodenum. Some people interpret this feeling as hunger because eating brings relief.
Many people with duodenal ulcers report pain that awakens them at night. This can also occur with jejunal ulcers. Jejunal pain will be a little lower, closer to your belly button. If you have an esophageal ulcer, it might feel like heartburn, which peaks at night.
Other possible symptoms related to peptic ulcer disease include:
- Bloated stomach.
- Burping or belching.
- Loss of appetite.
- Nausea and vomiting.
Symptoms of complications
Some people don’t have symptoms until peptic ulcer disease causes extra complications. This can happen when it goes untreated for too long. Untreated ulcers may begin to bleed or may continue to wear through your GI tract until there’s a hole.
Symptoms of upper gastrointestinal bleeding may include:
- Blood in your stool (poop).
- Black, tarry stool.
- Coffee ground vomitus.
- Dizziness or faintness.
- Pallor (paleness).
- Rapid heart rate.
Symptoms of a gastrointestinal perforation (hole) may include:
- Sudden, sharp and severe abdominal pain.
- Abdominal swelling and tenderness to touch.
- Fever and chills.
If you have untreated peptic ulcer disease for a long time, ulcers may continuously heal and then start again. Some people develop so much scarring and/or swelling from untreated ulcers in their GI tract that it can slow or stop food from moving through.
Symptoms of a gastrointestinal obstruction may include:
- Abdominal bloating, swelling and pain.
- Nausea and vomiting.
- Loss of appetite and weight loss.
- Loss of bowel movements and constipation.
What causes peptic ulcer disease?
The mucous lining in your gastrointestinal tract is designed to withstand digestive acids and enzymes and repair itself from damage, especially in your stomach and duodenum. Peptic ulcer disease occurs when something interferes with these natural defenses.
It takes a chronic or persistent condition to lower these defenses long enough for an ulcer to erode all the way through the mucous lining in your stomach or duodenum. Scientists have identified two main causes that account for almost all cases of PUD:
- H. pylori infection. Nearly half of the world’s population has this common bacterial infection living in their stomach and/or duodenum. In most people, it doesn’t seem to cause any trouble. But if it overgrows too much, upsetting the natural balance of microbes living there, it can invoke an inflammatory response. Chronic inflammation in your gastrointestinal lining can wear it out and diminish its resources for self-repair. The bacteria may also actively attack the lining.
- Overuse of NSAIDs (nonsteroidal anti-inflammatory drugs). NSAIDs are common over-the-counter (OTC) pain relievers, including aspirin and ibuprofen. Since you can get them without a prescription and take them without professional healthcare advice, it’s common for people to take too many, too often. This can affect the chemistry inside your stomach and duodenum. NSAIDs inhibit the prostaglandins that repair damage to your gastrointestinal lining.
Other uncommon causes of peptic ulcer disease include:
- Other infections.
- Ischemia (loss of blood supply).
- Severe physiological stress (usually from a life-threatening disease or injury).
- Chemotherapy or radiation therapy.
- Zollinger-Ellison syndrome.
- Crohn’s disease.
- Stomach cancer.
You can get a peptic ulcer in your jejunum, the middle part of your small intestine, if you have gastric bypass surgery that attaches your stomach directly to your jejunum. This effectively makes your jejunum your new duodenum, but without the same protective lining.
You can get a peptic ulcer in your esophagus if chronic inflammation (esophagitis) wears the lining down. Chronic acid reflux is the most common cause of chronic esophagitis, but there are others, including infections, medications and autoimmune diseases.
What are the risk factors for developing peptic ulcer disease?
You’re more likely to get peptic ulcer disease if you have an H. pyloriinfection or use NSAIDs regularly, especially if you have both risk factors. Even if H. pylori hasn’t overgrown yet or you haven’t taken too many NSAIDs yet, these factors can combine to cause PUD.
Other factors that may contribute include smoking, alcohol use and other medications you might be taking. While these factors aren’t enough to cause PUD all on their own, they can combine with H. pylori infection or NSAID use to make peptic ulcer disease more likely.
Diagnosis and Tests
How is peptic ulcer disease diagnosed?
If your symptoms and/or risk factors suggest peptic ulcer disease, a healthcare provider will look for the ulcer in your GI tract. They’ll also want to test you for an H. pylori infection. They might test for these separately or together during an endoscopy exam.
Detailed imaging tests, like a CT scan (computed tomography scan) or GI series X-ray exam, can detect larger ulcers. Tests for H. pylori infection include a urea breath test or a stool test. You might have some of these tests while your provider is evaluating your symptoms.
For many people, an upper endoscopy exam will provide the final diagnosis. An upper endoscopy (or EGD test) goes inside your upper GI tract with a tiny camera on the end of a long tube. During an endoscopy, they can also take a stomach biopsy to test for H. pylori.
Endoscopy is helpful because it doesn’t just show images of your organs, but also allows your provider to access them directly by passing long instruments through the tube. If your ulcers need treatment to stop bleeding, they can treat them on sight.
Management and Treatment
What are the available treatments for peptic ulcer disease?
First-line treatment for peptic ulcer disease is a combination of medications to reduce gastric acid and help protect and repair your tissues. You’ll also need antibiotics if you have an infection. It’s important to eliminate the underlying cause of your ulcer.
Medications are enough to treat most peptic ulcers, but you might need additional treatment if you have complications, like a bleeding ulcer or perforated ulcer. Minor medical procedures, like endoscopy, can treat most of these complications.
Medications
Peptic ulcer medications include:
Antibiotics. If you have an H. pylori or other bacterial infection, your healthcare provider will prescribe some combination of antibiotics to kill the bacteria.
Common antibiotics for H. pylori infection include:
- Doxycycline.
- Metronidazole.
- Clarithromycin.
- Amoxicillin.
Cytoprotective agents. These medicines help to coat and protect your gastrointestinal lining while it heals. They include:
- Sucralfate.
- Misoprostol.
- Bismuth subsalicylate.
Histamine receptor blockers (H2 blockers). These drugs reduce stomach acid by blocking the chemical that tells your body to produce it. They include:
- Famotidine.
- Cimetidine.
- Nizatidine.
Proton pump inhibitors (PPIs). These drugs help reduce stomach acid and also coat and protect your mucous lining to promote healing. PPIs include:
- Esomeprazole.
- Dexlansoprazole.
- Lansoprazole.
- Omeprazole.
- Pantoprazole.
- Rabeprazole.
NSAID alternatives. If you usually take NSAIDs, you’ll need to discuss alternatives with your healthcare provider. Acetaminophen is one common over-the-counter pain reliever that’s not an NSAID and doesn’t have the same effects on your mucous lining.
Medical procedures
If you have a complicated or bleeding ulcer, your provider may need to treat it directly. They can usually do this during your endoscopy exam. Providers treat bleeding by cauterizing or injecting medication into the wound. They’ll repair a perforation with stitches.
If an ulcer causes an obstruction in your duodenum or your pyloric channel (the outlet at the bottom of your stomach), you might need interventions to reopen the channel. This might mean suctioning your stomach to decompress it or, rarely, surgery.
Prevention
How can you lower the risk of peptic ulcers?
The most important things you can do to prevent peptic ulcer disease are to:
- Find and eradicate H. pylori. Most people who have an H. pyloriinfection aren’t aware of it. You can find out if you have it by taking a simple urea breath test. If you have it, you can treat it proactively (before it causes any problems). If you’ve had it and treated it before, it’s a good idea to retest because sometimes it comes back.
- Use NSAIDs only as directed. If you’re in the habit of managing daily aches and pains with NSAIDs, make sure you aren’t taking more than the recommended dose. If you’ve already had peptic ulcer disease, you probably shouldn’t take them at all. But if you have to, you should take them with another medication to protect your lining.
Prognosis/Outcomes
Do peptic ulcers go away on their own?
Peptic ulcers can heal if the conditions that caused them go away. But it usually takes a medical diagnosis to identify the cause. And if the cause is an H. pylori infection, or some other medical condition, you’ll need treatment to make it go away.
If the cause was NSAIDs alone, and if you’ve stopped taking them, your ulcer might heal by itself. But you’ll need a medical diagnosis to make sure. You could have H. pylori also, and NSAID use could allow a previously harmless infection to overgrow.
What is the prognosis after treatment for peptic ulcer disease?
Most peptic ulcers heal within a few weeks. Most people will only need medication for about two months. Medications are very effective in treating peptic ulcers. People with chronic conditions, like Zollinger-Ellison syndrome, may need to take them for life.
Your healthcare provider will conduct follow-up tests after treatment to make sure the ulcer has healed, and any infection has cleared. H. pylorican be tricky, and sometimes it comes back. Ulcers can also come back if the conditions that caused them continue.
Rarely, some people have persistent stomach ulcers that don’t respond to treatment or that keep coming back after treatment. They can cause chronic pain, excessive scarring and other complications. These cases might require surgery to:
- Remove scar tissue or open up the outlet (pyloroplasty).
- Sever the nerve that triggers stomach acid (vagotomy).
How to live with Ulcers?
Adjust your diet while living with peptic ulcer disease.
Foods and drinks don’t cause peptic ulcers, but they can aggravate them if you have them, especially spicy and acidic foods and drinks. You should also avoid alcohol and smoking if you have symptoms or a history of peptic ulcer disease.
You need to adjust your medications while living with peptic ulcer disease.
Make sure to discuss all of your current medications with your healthcare provider. NSAIDs are the most important to discuss, but other medications can also contribute, especially when combined. You may need to find alternatives or adjust your dosage.
Can I treat peptic ulcer disease with antacids at home?
Antacids help to neutralize acid and reduce symptoms related to acid, like reflux, heartburn and indigestion. They might make an ulcer feel better, but they can’t cure it. If you have a history of peptic ulcers, antacids might help prevent them from recurring.
When should I call my healthcare provider?
Always see your provider if you suspect you have a peptic ulcer. While you may be able to manage your symptoms temporarily with over-the-counter medications, these won’t heal the ulcer. You need to identify and address the underlying cause.
An untreated ulcer can lead to serious complications, even if you don’t have severe symptoms. The major cause of peptic ulcer disease, H. pylori, can also lead to other complications. For example, it’s a risk factor for developing stomach cancer.
Seek emergency care if you develop symptoms of serious complications, like:
- Severe pain that doesn’t go away.
- Signs of blood in your poop or bloody vomit.
- Signs of severe blood loss, like paleness and faintness.
A note from Toptee Healthcare Plus
Peptic ulcer disease represents a significant change inside your GI tract. Something has overcome your natural defenses against stomach acids and enzymes. This chemical change takes time to develop, and it usually takes medical treatment to fix.
Peptic ulcers are common and treatable, but treatment is important, even if you don’t have severe symptoms. Untreated ulcers can continue to deepen until they become more serious. Don’t wait to consult your healthcare provider about your symptoms.